Why Spinal Mobility Isn’t Helping Low Back Pain
2023-01-2
To be honest, it made sense to me as well. When I was first having low back issues at 14 and was in physical therapy, I was told to stretch, stretch, and stretch. Admittedly, it felt good at the time, but I would become tight just a few hours later and have low back issues once again.

That is why when people in the fitness industry claim that the solution to low back pain is more spinal mobility training, they are right and wrong at the same time. How can that be?
The Wrong
People often think that if we are having low back pain it is because our spine isn’t mobile. You can find studies like the following that say, “In summary, we found that a restriction in lateral flexion and hamstring range of motion as well as limited lumbar lordosis were associated with an increased risk of developing low back pain”.
Well that is it right?! If we can’t move our spine and have tight hamstrings we have to add more spinal mobility and stretching our hamstring more right? Not quite.
What studies like this tell us is that we should have freedom of movement in our body and when we do not we are at risk for developing issues like low back pain. However, the idea that the reason our body is “tight” is due to muscular tightness and joint dysfunction is not really accurate.
This 2018 study really points out some important keys to understand, “Pathological mechanisms of discogenic low back pain include sensory nerve ingrowth into inner layers of the intervertebral disc, upregulation of neurotrophic factors and cytokines, and instability. Inhibition of these mechanisms is important in the treatment of discogenic low back pain.”
Let us start with the easiest, study after study actually shows those with mechanical low back pain have TOO much instability of the intervertebral segments causing disc and potentially nerve issues as well. In reaction to this instability the nervous system “reacts” by creating tightness in the body because it wouldn’t be good from a survival stand point to have our spine that is already unstable to create more and more movement.

This study showed how the low back pain group (in black) had MORE movement of the spine that those without low back pain.
To be honest, we could probably do A LOT of good for low back pain with just THIS realization, however, there is something else that I think one of the studies brought up that is fascinating to look at and has been collaborated and being discussed by other research studies. That is cytokines in the blood stream and its relationship with low back pain.
Now, what are cytokines? “A type of protein that is made by certain immune and non-immune cells and has an effect on the immune system. Some cytokines stimulate the immune system and others slow it down.”(National Cancer Institute)
I’m not going to pretend I’m an expert in cytokines, but what has been interesting to see is that many studies have found that a high level of cytokines can often be present when we also see chronic low back pain. Researchers often make a rather logical leap that this is due to the inflammation that is going on in the body during chronic states of pain (that can cause a host of issues themselves having the body being in appreciable inflammation for long periods of time).
Well, how can we help reduce the cytokines we are seeing and even other stress hormones like cortisol? Glad you asked;)
The Right
So, going to answer our cytokine and instability issues in a moment, but wanted to address what we have right about low back pain and mobility. The key is that the lack of range of motion we often see in spinal movement isn’t about the spine itself, but LACK of stability of the spine which causes reduction in hip mobility which does have a huge impact upon our low back pain.
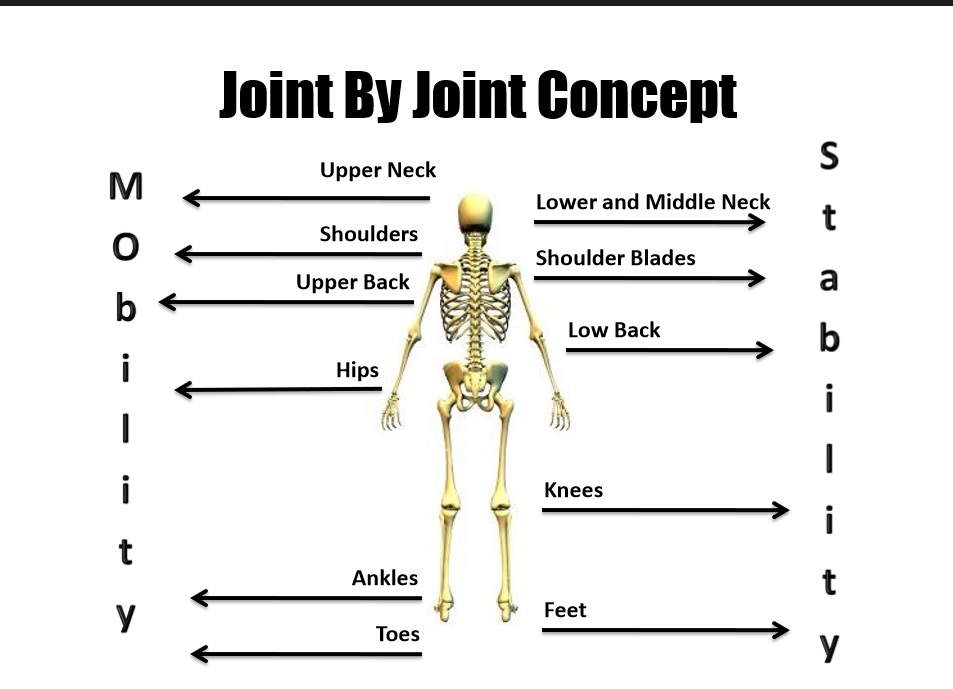
The joint by joint model is an easy way to understand how instability of the core/lumbar spine causes tightness to occur not just at the hip joint, but in the muscles like the psoas and hamstrings as well.
However, what should be becoming clear is not that we should just stretching more, but we need a combination of movement based stretching, stability, motor control, and learning how to take off the brakes. The idea I came up with was inspired by research like the 2012 study that found HUGE improvements in mobility could be improved without any isolation of the muscles or joints.

What is myofascial stretching though? We know that our body is a series of chains often connected by fascia. It makes sense that we don’t actually just stretch muscles (in fact, it can be fascia that is more problematic than muscle) and to really see significant changes in our movement and mobility we would encompass fascia, muscle, and joint movements which myofascial systems try to employ.

“A more thorough stretch would be obtained if stretching included not only hip joint motion but also the entire side of the body which was under stretch at the hip, thus incorporating some of the principles of myofascial force transmission (12,13,23,30,34). For example, stretching of the right hip internal rotation would also include elevation of the right arm overhead, with extension and left side bending of the torso . Stretches were performed in a position approximating upright posture.”
So, before I give you some ideas on much BETTER ways to improve low back pain and our mobility what about those darn cytokines?! Did you forget? The idea is that signs of such proteins and cortisol often found in chronic pain individuals shows our body is almost constantly stressed in these conditions. That is why mind-body systems like yoga and qigong have actually shown in research to decrease both cytokines and cortisol. Reducing the stress response of the body can actually change how our brain perceives our pain as well. Overall allowing us with good movement to enhance our well being in more effective ways.
Don’t miss the final week to get our early bird pricing on our 4-week live online Myofascial Integrated Movement low back pain masterclass HERE and save 25% on all other DVRT functional training tools, workout programs, and courses/certifications HERE with code “fall25”
I know, you don’t want to become a yoga guru or a qigong master, I get it! You don’t have to! Taking principles and concepts along with blending modern science of the body can make short practices very effective. I should know as it has totally changed how my body feels with a pretty significant disease and why I want to share strategies like these with you! Check out some of the ideas below and find out MUCH more in our Myofascial Integrated Movement program HERE
© 2026 Ultimate Sandbag Training. Site by Jennifer Web Design.